Pharmacy
We’re here to help you get the most out of your medicine cover, without the confusion.
Managing your medication doesn’t need to be complicated. Whether you need a once-off script for something short-term, ongoing treatment for a chronic condition, or help understanding what’s covered, we’re here to guide you every step of the way.
In this section, you’ll find everything you need on acute and chronic medicine benefits, how to apply for authorisation, which medicines are on the formulary and how to use your pharmacy network to avoid unexpected costs and co-payments.
Our goal is to take the uncertainty out of your pharmacy benefits so that you can focus on your health, not the paperwork.

Acute medication
Short-term treatment made simple—know what’s covered and how to avoid unexpected costs.
Your acute medication benefit covers treatment prescribed by your doctor for short-term or occasional use—like antibiotics, pain medication, or allergy relief. This includes both once-off prescriptions and repeat courses.
No authorisation needed: Just take your valid script to your nearest network pharmacy and they’ll submit the claim for you.
To make the most of your benefit and reduce out-of-pocket payments:
- Choose cost-effective generics—your pharmacist can guide you.
- Check your benefit limits to make sure you have enough cover available.
- Always use a network pharmacy to avoid additional dispensing fees.
ℹ️ Note: Some long-term treatments may be funded from this benefit if your condition isn’t listed on your Schemes approved chronic condition list.
Disclaimer: Scheme rules will always apply. The Acute Medication Benefit is subject to applicable quantity limits, rand limits, member co-payments or levies, formulary or reference pricing, and specific exclusions.
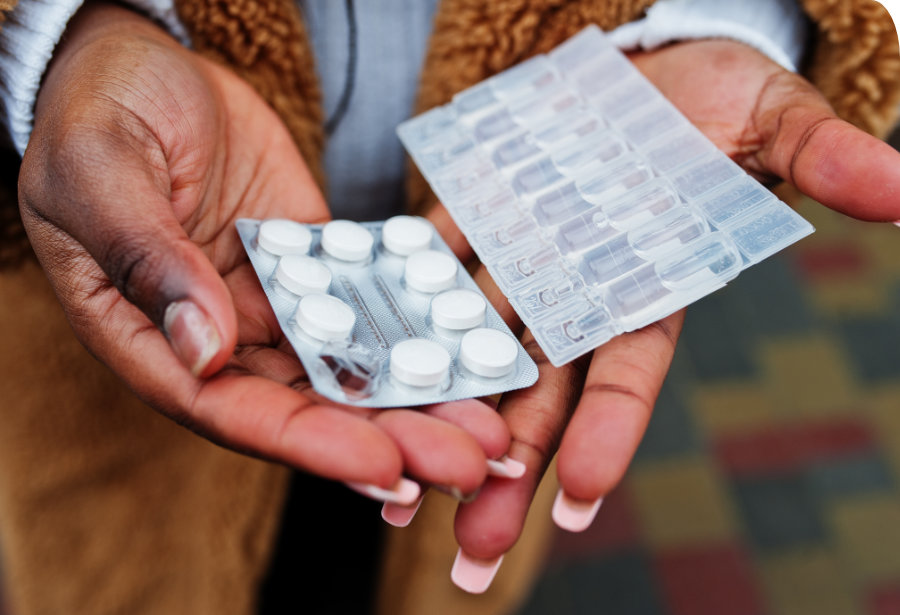

Chronic medication
Apply for ongoing treatment of chronic conditions like diabetes, hypertension, or asthma and get the support you need, long-term.
If you’ve been diagnosed with a chronic condition that’s covered by your Scheme, your treatment may be funded from your chronic medication benefit.
Not all long-term medicines qualify for this benefit, so it’s important to check what’s covered. Your Scheme provides unlimited coverage for all listed Prescribed Minimum Benefit (PMB) conditions, as well as an unlimited benefit for additional listed chronic conditions.
➡️ Check your Schemes list of approved chronic conditions before applying.
Make the most of your chronic medication benefit
- Register your condition by completing and submitting a chronic application form before taking your script to the pharmacy.
- Ask your doctor to prescribe from the chronic medicine formulary to avoid funding issues or co-payments.
- Review your chronic authorisation letter carefully—it may include additional information like the dates for which the medicine is authorised, any required documents (like lab tests) that still need to be submitted to the Scheme, or authorisation renewal conditions.
- Speak to your pharmacist about using cost-effective generics.
- Visit a network pharmacy to avoid additional fees and get help managing your treatment.
If any items aren’t covered in full, speak to your doctor about more affordable alternatives that are still clinically appropriate.
Understanding the Authorisation Amount (Chronic Drug Amount – CDA)
When your chronic medication is approved, it is funded up to a maximum amount known as the Chronic Drug Amount (CDA). This amount is set per drug category and is based on clinical guidelines and the cost of all recognised treatment options.
- The CDA excludes the dispensing fee and reflects the highest amount your Scheme will pay for the medicine.
- If the cost of your medicine is higher than the CDA, you’ll need to pay the difference.
- The CDA is reviewed regularly and may change with market pricing.
💡 Tip: Stick to formulary items and ask for generics to stay within your CDA and avoid out-of-pocket costs.
Chronic Application Checklist
Here’s what you’ll need to register your condition and start claiming from the benefit:
✅ Step 1: Complete the Application Form
- Ask your doctor to complete the Chronic Medicine Application Form, including all the relevant sections for your condition/s.
- Ensure it includes:
- Diagnosis (ICD-10 code)
- Prescribed medicine (name, dose, frequency of use)
- Supporting tests or motivations, if required
- Doctor’s details and signature
✅ Step 2: Confirm the Condition is Covered
- Refer to your Scheme’s benefit guide to check if the condition is listed
✅ Step 3: Submit Your Application
- Ask your network pharmacy to send it on your behalf, or
- Email it directly to your Scheme (check the form for contact details)
✅ Step 4: Wait for Authorisation
- You’ll receive an authorisation letter showing:
- Approved medicines
- Valid dates
- Any additional requirements
❗Don’t fill your script until you’ve received approval.
✅ Step 5: Collect Your Medicine
- Take your script and authorisation letter to a network pharmacy
- Ask for generics and formulary items to reduce or avoid any co-payments
✅ Step 6: Keep Your Authorisation Updated
- Submit a new script before your authorisation expires
- Send in any updated tests or documents required by your Scheme
- Update your authorisation if your treatment changes
💡 Tip: You only need to submit a new script if you are diagnosed with a new chronic condition covered on your Scheme, your authorised medicine for your current condition has changed in any way or your medicine authorisation has an expiry date.
Chronic Disclaimer: Scheme rules apply. The Chronic Medication Benefit is subject to applicable clinical protocols and entry criteria, member co-payments or levies, formulary or reference pricing and specific exclusions.
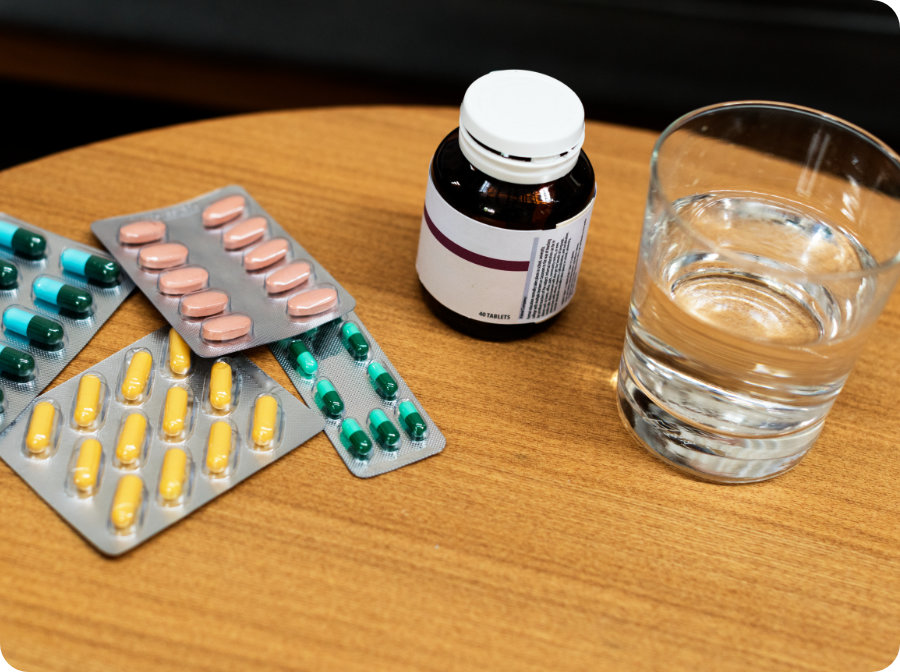

Over the counter (OTC) medication
Get quick relief with cover for self-medication—no prescription needed.
Your Scheme includes a benefit that pays for medication you can buy without a doctor’s prescription from a pharmacy. This typically includes everyday items like cold and flu treatments or mild painkillers.
Make the most of your OTC cover
- Check your available limit—this limited benefit is capped by a set amount per script.
- Visit a network pharmacy to ensure your claim is processed correctly.
- Ask for generics to make your benefit go further.
No formulary applies, but general scheme exclusions still apply—certain items (like supplements or beauty products) may not be covered.

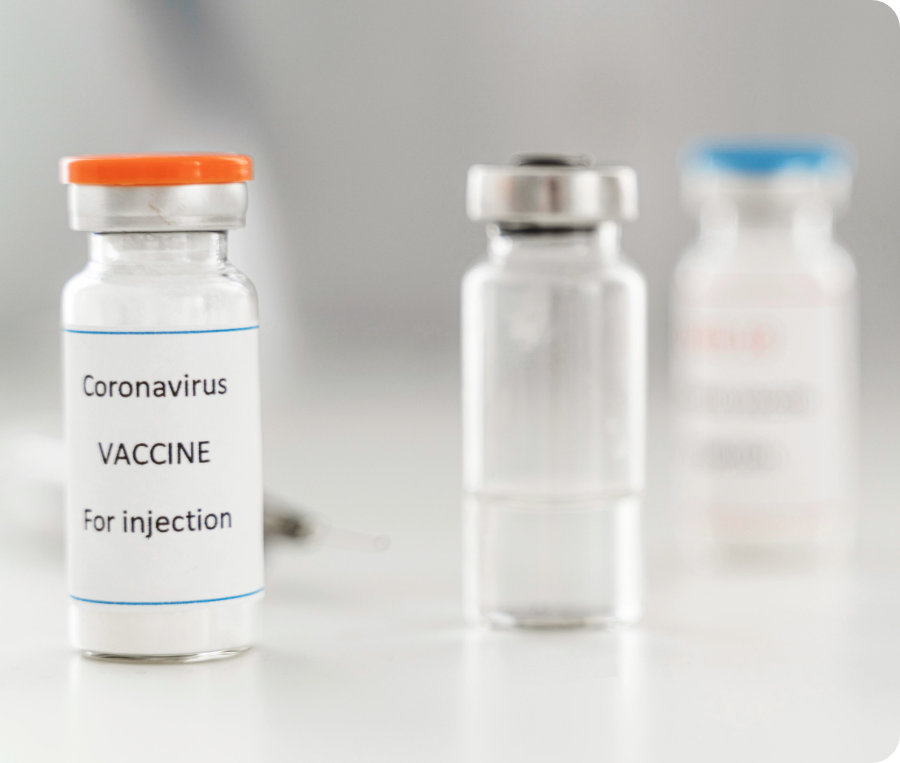
Vaccines
Vaccines work by preparing your immune system to recognise specific viruses or bacteria. This allows your body to respond quickly and effectively if you’re exposed in future, helping to prevent serious illness.
List of childhood and other vaccines covered by your Scheme.
Medicine Formulary
Find approved medicines covered by your Scheme.
A formulary is a list of medicines your medical scheme covers based on clinical guidelines, cost-effectiveness and availability.
Your Scheme has a custom list of medications designed to match its benefits.
To help you get the most out of your cover and avoid extra costs, your doctor should prescribe from this list whenever possible.
Why the formulary matters
- Medicines on the formulary are usually funded in full if entry criteria are met
- ⚠️ Out-of-pocket costs: If your prescribed medicine isn’t on the list or exceeds reference pricing, you may need to pay the difference.
How to avoid unexpected expenses
- Check the formulary before filling your script.
- Ask your doctor to prescribe listed alternatives when needed.
- Speak to your pharmacist about generics if your brand-name medicine isn’t covered in full.
- Use a network pharmacy to ensure correct pricing and claim submission.
💡 Tip: If a medication you need isn’t on the list, your doctor can submit a motivation for clinical review, but this isn’t guaranteed to be approved.
Disclaimer: Scheme rules, entry criteria and reference pricing will apply. Medicines outside the formulary may attract co-payments or be excluded, depending on your plan.
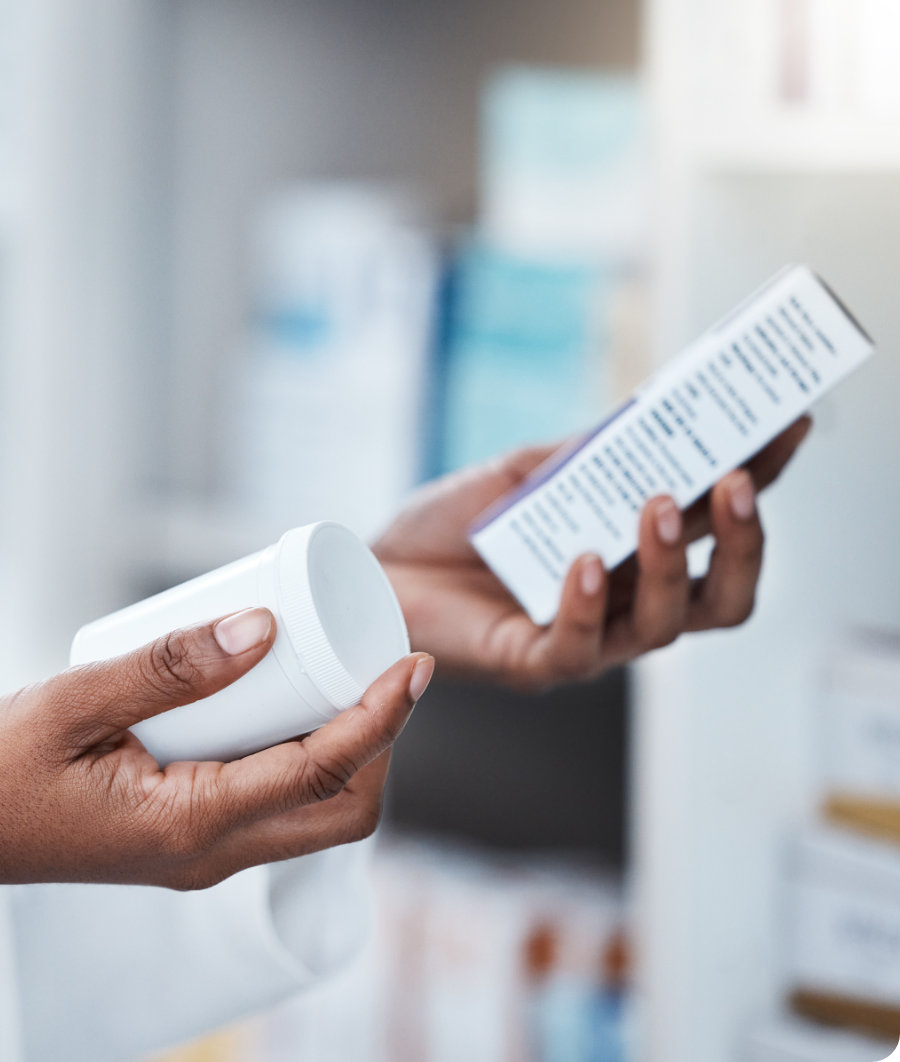
Network pharmacies
Find a network pharmacy near you. Network pharmacies charge within the scheme rates, helping you avoid out of pocket expenses.
Your Scheme partners with a network of pharmacies that charge within scheme-approved rates. This helps you avoid unnecessary out-of-pocket expenses and ensures your claims are processed correctly the first time.
Network pharmacies can help you with:
- Chronic authorisation applications – they’ll assist with submitting the right forms.
- Generic substitution – they can recommend lower-cost alternatives to help you stay within your benefits.
- Ongoing chronic care – they support you in staying compliant with your treatment so you can better manage your condition over time.

